If you’re wondering whether you should utilize artificial intelligence for medical billing products, the short answer is yes. The demand for such products is growing steadily.
Let’s see the numbers to confirm that. According to the data from the Bureau of Labor and Statistics, the medical billing and coding field was expected to grow 7 percent from 2021 to 2031. This means that about 14,900 new jobs will open each year.
At the same time, medical billing and coding workers still experience certain industry-related challenges while trying to handle all the healthcare data precisely. The more overwhelmed with the amount of this data they are, the higher the chances of errors.
Luckily, AI is here to help — and we are here to tell you how exactly. Mind Studios has been providing custom healthcare development services worldwide for over 10 years already. Through that time, we’ve been exploring and utilizing the latest trends, with AI technologies being no exception.
In this article, we want to share our knowledge with you and offer some reasons to start implementing such solutions in your medical billing products.
The modern challenges in medical billing

Medical billing has its challenges that, if not addressed properly, could cause staff burnout and worsen the patient experience. Let’s learn more about the most common challenges and how using AI in medical billing can help solve them.
Coding issues
Accurate coding and documentation is a must-have when you want to create clean claims. However, these processes are mostly handled by humans these days — and humans can make typos and errors. While these things might not seem significant at first glance, even a small typo could lead to claim denial.
Combining medical coding and artificial intelligence can help human coders do their job quicker and reduce the risk of errors. This is already done by ProSciento, who adopted the IBM Clinical Development Medical Coding with Watson AI technology. The result could read an unstructured text and automatically generate appropriate code suggestions. This allows medical coders to code 84% of terms using no more than one search. This helps ease their fatigue and frustration, as well as increase efficiency.
Updating patient information on time
Keeping patient information up-to-date is critical for medical institutions. Not only it allows healthcare professionals to suggest more accurate and relevant treatment but also reduces the risk of claim denial — as clean claims require accurate patient information.
Using AI in medical billing helps update patient data quicker. Some solutions like Regard do it automatically, reducing burnout among healthcare workers. Other solutions like Viz.ai offer cloud-based patient record management systems that share information quicker. In this case, when a patient changes something in their electronic health record (EHR), the medical institution receives the update instantly.
Tracking denials and resubmitting them
In 2022, the claim denial rate reached 11%, according to Crowe. Furthermore, not all the denied claims are actually resubmitted. The reasons for that can be very different, from missing documentation to inaccurate patient information.
AI-powered solutions can help change that, using analytical tools to help providers predict and prevent denials, as well as process them. Such a solution is already developed by Experian Health. It operates before the claim submission, spotting and editing claims with a high risk of denial. It also steps in if a claim has been denied, identifying the ones that can be potentially reimbursed.
Types of Artificial Intelligence in medical billing
AI in medical coding and billing comes in many forms, the most popular of them being machine learning, natural language processing, and computer vision. These technologies can be utilized either separately or in combination with each other to optimize and simplify medical billing processes.
Machine Learning
Machine learning is a form of AI that uses data and algorithms to train digital systems. This is similar to how humans learn, only the number of data, in this case, is much bigger.
With the help of ML, digital systems learn which billing codes are associated with specific medical tasks. This makes the job of software engineers much easier as now they don’t need to write a rule for every possible medical intervention manually.
Natural Language Processing
Similarly to ML, natural language processing (NLP) also trains software — in this case, to understand the raw human language. By default, digital systems cannot process unstructured information. But with the help of NLP, they become able to not only understand it but also translate it into meaningful data. For instance, it can be used to help systems read healthcare professional notes more accurately and assign correct codes to them.
Computer Vision
This AI technology is used to help digital systems recognize data on images, such as presentations, scanned notes, PDFs, and so on. With the help of Computer Vision, digital systems become able to quickly process and understand key data in EMRs, billing software, and insurer web portals.
How AI is used in medical billing systems
So what exactly are those AI types used for? Let’s look at some use cases:
Increased efficiency in claims processing
Using AI technologies for medical billing automation can help ease the struggles of medical coders working hard to assign codes accurately and, in turn, speed up the claims processing and increase its efficiency. Error checking, patient eligibility verification, and claim submitting — all of these can be easily done with the help of AI-powered tools.
Detection of fraudulent claims
The ability to quickly process big chunks of data and spot certain patterns can help AI solutions in fraud prevention. If they are trained to identify potential fraud, abuse, and waste, they can do it quicker than human workers.
Reduction in billing errors
Medical billing errors are one of the main reasons for claim denial. Such denials aren’t only inconvenient to patients but also cause financial losses to healthcare providers. Using AI for medical billing analysis can help reduce the number of those errors, optimize payment schedules, and minimize those losses.
Improved revenue cycle management
Revenue cycle management is a complex process that consists of lots of different factors:
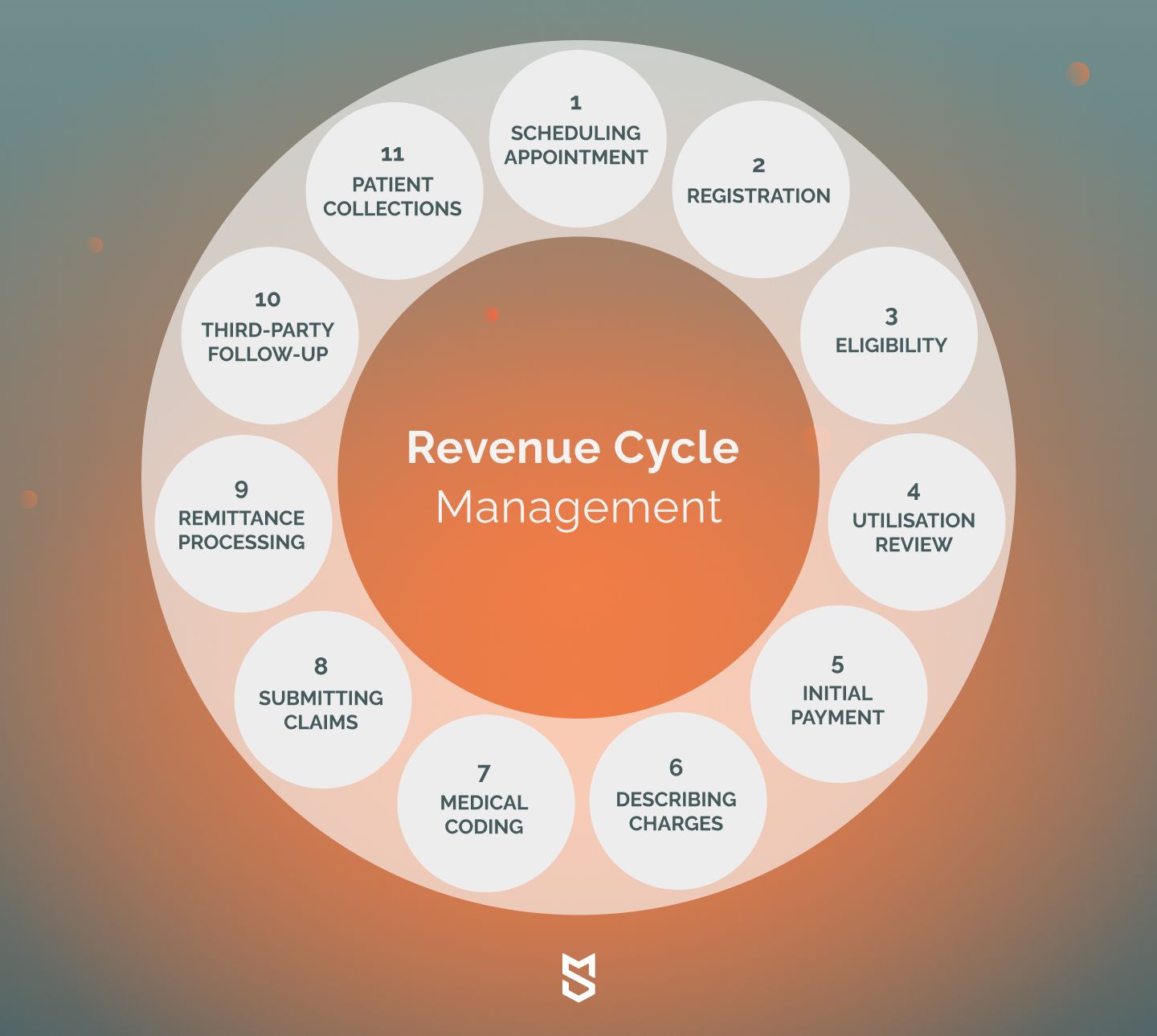
So if there’s a possibility to simplify it by utilizing AI solutions, why not give it a try? One of the easiest ways to do that is to create AI-powered chatbots that can help with:
- patient registration and eligibility verifications
- claims processing
- coding and billing services
- collection of payments
AI can also automate follow-ups on claims that have been either denied or not paid, as well as offer payment reminders and other important notifications.
The limitations of AI in medical billing

One of the common fears of medical staff is being replaced by AI technologies. However, that’s not likely to happen in the near future. Although AI and medical billing can be well combined, it’s still important to remember that this technology, being relatively new, has its limitations. Here are the most common of them.
Dependence on high-quality data
On one hand, implementing artificial intelligence in medical coding and billing can help lower the risk of human error. On the other hand, AI technologies can make mistakes too.
Why so? Because they are trained using various data. If the data used to train them is of low quality and contains errors or misleading information, AI technologies can come to the wrong conclusions.
Data sharing
Artificial intelligence software in medical billing doesn’t operate in a vacuum. It has to share various data with different organizations. However, this is where the challenge starts.
At the moment, various healthcare businesses operate on systems that use different formats of data. That’s why it’s harder to sync such data: there’s always a chance that your preferred data format might not be supported by the tools your partners use.
Ongoing learning
Just like a person who needs to hone their skills and knowledge to grow professionally, artificial intelligence in medical billing also needs to continue learning. After all, the data updates and changes as time goes on, and in order to remain efficient and relevant, AI technologies need to analyze this new data.
This means that we need to set up a neural network capable of analysis and ensure that only up-to-date, relevant data is used to continue training it.
Regulation standards compliance
As medical institutions are dealing with very sensitive data daily, it’s essential to ensure that this data is truly secure in their hands. To achieve that, the healthcare industry uses a set of regulations and standards such as HIPAA.
While not all healthcare application development has to meet these requirements, the apps that use patients’ personal and financial information definitely should. Unfortunately, at the moment, most AI solutions aren’t HIPAA compliant.
Human supervision
Last but not least, while AI technology can help healthcare professionals automate routine and repetitive tasks, it still needs human supervision when it comes to more complex duties and communication. Furthermore, not all patients feel comfortable having dialogues with AI that, at the moment, don’t have the interpersonal skills that humans possess.
All of the above only proves that currently, AI technologies cannot deliver all the work alone without human supervision and support. Instead, they can make the lives of healthcare professionals much easier by offering solutions for automated medical billing. As a result, people can focus on the tasks that require more personal input and let AI handle the rest.
If you’re looking for ways to speed up your working processes with the help of AI, Mind Studios can help you with that. We’ve been providing healthcare software development services for years and know all about its nuances. We can utilize that knowledge to help you train and integrate an AI technology of choice into an existing project, as well as offer you some valuable suggestions based on our experience.
Conclusion
AI technologies are here to stay. Knowing that, it’s only natural to try and figure out how they can benefit your industry and your particular project.
When it comes to medical billing, AI tools can help you avoid fraudulent claims, reduce billing errors, make the claim processing more efficient, and do other things that help your employees save time and nerves, and your company save money.
Being a company with vast experience in the niche, Mind Studios can offer you our help in picking the right AI technology for your needs, training it, and implementing it in your project efficiently. Get in touch to receive valuable insights and start working!